Definition: Dysplasia of the corneal epithelium refers to abnormal maturation of the epithelium as it differentiates from the basal layer in the superficial layers. Rarely, primary intraepithelial neoplasia may arise in the cornea.
Epidemiology: The incidence of dysplasia, carcinoma in situ, and invasive carcinoma of the cornea and conjunctiva was estimated to be 1.9 per 100,000 per year averaged for 10 years in a study from Brisbane, Australia. In a study from Queensland, Australia, 288 cases were identified 155 dysplasia, 71 carcinoma in situ, 62 squamous cell carcinoma. 78.5% of the cases occurred in males with an average age of 60.1 years. Squamous cell carcinoma was found to be most prevalent in the limbal region.
Etiology: precancerous lesions associated with dysplasia often appear in conjunction with preexisting pinguecula within the epithelium. Their development is strongly correlated to overexposure of the conjunctiva to ultraviolet light. The appearance of dysplasia has also been associated with human papillomavirus type 16 (HPV16). HPV is associated with bilateral conjunctival tumors manifested as multiple lesions of the tarsal and bulbar conjunctiva. In addition to these tumors, invading dysplasia and squamous cell carcinoma has been found in the eyes of patients harboring this disease. HPV 16 is also present in benign squamous papillomas (75%) in some series so that the role HPV 16 infection alone, in producing dysplasia has been questioned.
Clinical Findings:Patients often present with irritation, reported in 40% of the cases. Dysplasia usually appears as a diffuse, gelatinous, and semitransparent epithelium. Most lesions originate at the limbus. Untreated lesions often involve the palpebral fissure and protrude between the eyelids. Recurrences occur in about 23% of the cases in some series.
 Histopathology:
Histopathology: At low magnification the epithelium shows acanthosis, cellular crowding and altered cellular polarity without maturation. There is nuclear enlargement, dyskeratosis, and often mitotic figures above the basal layer of the epithelium. There may be pleomorphism and abnormal mitoses. Squamous cell carcinoma are defined by invasion of the substantia propria and vary widely in size and often exhibit surface keratinization and squamous eddies and pearls.
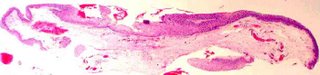
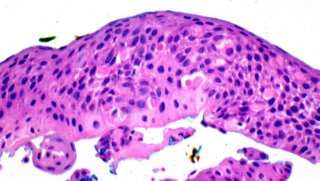 Treatment:
Treatment: Established treatment techniques include a careful excision using appropriate margins. Autografting may be necessary to close a large defect. Most small sized conjunctival intraepithelial neoplasia can be effectively treated with topical drops of
Mitomycin C. Cryotherapy as well as application of topical conjunctival chemotherapy with 1%
5-FU may also be used as an adjunctive therapy to treat incompletely excised or recurrent carcinomas. In a study of ten patients with recurrent squamous cell carcinoma (average age 66 years) the tumor response to
Mitomycin C was evaluated. Following six weeks of treatment cycles in which topical drops of .04%
Mitomycin C were administered to the eye four times per day, all ten cases showed tumor regression. No complications were documented. The efficacy of
topical 5-FU was also documented in a case study of eight patients with recurrent or untreated squamous cell carcinoma. The application of 1%
5-FU eye drops four times daily for four weeks resulted in clinical regression for all 8 patients. After three months the complete recovery of normal epithelium was observed in all cases with no long-term side effects.
References: Lee, GA Australian NZJ Opthamology 1997(4): 269-76
Spencer, Ophthalmic Pathology. W.B> Saunders Company, 1996(1): 113-115.
Shields CL, Am Journal of Ophthalmology 2002(5): 601-6
Edoardo Midena, Claudia Degli Angeli, Massimo Valenti, Valentina de Belvis, Paolo Boccato, Br Journal of Ophthamology 2000(84): 268-272