Definition: PHPV is a congenital condition with persistent hyaloid vasculature and mesenchymal tissue from the embryonic primary vitreous in a microphthalmic eye. It is often seen in combination with other syndromes. The syndrome has been renamed recently as persistent fetal vasculature.
Incidence/Prevalence: Rare. About 50 cases were seen in a busy pediatric referral surgery practice over 10 years (Ref 2).
Etiology: Described by Reese in 1949, PHPV is thought to be congenital. As the ectoderm of the lens plate and neuroectoderm of the optic vesicle separate, vasoformative mesenchymal tissue normally grows in to the space. In PHPV the tissue is thought to persist, hence the name. Recently it was discovered that mice lacking a tumor suppressor gene (Arf) have an anomaly similar to human PHPV. (
Ref 1) PHPV has been described in association with neurofibromatosis 2 and Axenfeld-Rieger syndrome with its concomitant chromosomal abnormality.
Clinical Findings: The disease may be either unilateral (90%) or less commonly bilateral (10%). The patient usually has leukocoria, markedly reduced vision and a small eye.
Gross: The earliest or most mild findings are elongation of the ciliary processes and the eye may be normal in size. In more severe cases the eye is small (as shown in the figure).

There may be an accompanying retinal detachment that is considered by most to be tractional. In the figure there is clearly blue subretinal exudate that fills the vitreous cavity around the retinal detachment (arrow 1). In most cases, fibrovascular or primitive vasoformative tissue (number 2) and mesenchymal tissue, including cartilage, mature adipose tissue and smooth muscle, arise from the primitive tissue behind the lens. Often times a hyaloid vessels is seen attaching to the mesenchymal tissue which is directly behind the lens. The mesenchymal tissue is attached laterally to elongated and centrally dislocated ciliary processes (arrow 3), a characteristic pathologic feature.
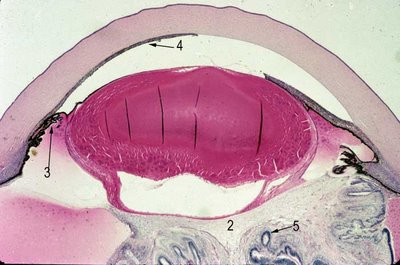
Retinal dysplasia may be seen in the retina behind the lens (arrow 5). Microophthalmia, cataract (here a generalized cortical cataract) and a variety of anomalies of the anterior chamber angle are seen with PHPV. In this figure the iris completely occludes the angle and trabecular meshwork with extensive peripheral and central (arrow 4) anterior synechiae.
Treatment: Lensectomy with or without anterior or total vitrectomy, and trabeculectomy are generally the procedures that are performed depending on the clinical presentation. The retinal detachment can be repaired. Attempts at early surgical rehabilitation prior to 77 days may have a better visual outcome. (
Ref 2)
References:
Thorton J.D. IOVS 2007Hunt A. BJO 2005.